
Ingabire sits with a child on her lap, now able to manage daily chores after receiving the medical care she needed—care that would have been nearly impossible without Mutuelle de Santé.
On most afternoons, Comfort Ingabire moves quietly around her family home in Karongi district, washing dishes, tidying rooms and revising her school notes. There is little to distinguish the 17-year-old from her peers, until her mother begins to tell the story of the fragile heart that once threatened to silence that ordinary rhythm of life.
Born at King Faisal Hospital, Ingabire entered the world with a congenital heart defect that went undetected until she was about two years old. Doctors discovered a hole in her heart, a diagnosis that left her mother, Betty Mbabazi, suspended between disbelief and fear.
“They told me my baby’s heart has issues about two years after her birth,” Mbabazi recalls, her voice steady but reflective. “At that moment, I did not know whether to cry or to pray. I was in total shock. But the only thing I knew was that I wanted her to live.”
For Mbabazi, that resolve quickly turned into a full-time commitment. As Ingabire’s condition became clearer, hospital visits multiplied. There were consultations, referrals and repeated examinations.
Mbabazi gradually put aside other responsibilities to become her daughter’s primary caregiver. What began as a mother’s instinct evolved into a demanding, unpaid occupation, monitoring symptoms, managing medication schedules and accompanying her child to every medical appointment.
Ingabire’s father, like her mother, is a farmer. The family depends largely on seasonal harvests, vulnerable to weather patterns and fluctuating market prices. There was seldom enough money to comfortably cover hospital bills, transport costs and medication.
Most times, they sold produce just to meet urgent medical expenses. Specialized cardiac surgery was far beyond the family’s financial reach. When doctors confirmed that Ingabire required advanced intervention abroad, the news felt overwhelming.
Yet community solidarity stepped in. Friends, extended family members and well-wishers mobilized contributions that eventually enabled Ingabire to travel to Germany at age five for life-saving surgery.
Her parents accompanied her with little more than hope and modest savings. Their own contribution covered only basic welfare expenses during the stay. The surgery itself was made possible through collective generosity.
The operation was successful, but recovery marked the beginning of a long, delicate journey. Her childhood unfolded differently from that of her peers. Growth was slow and physical development lagged behind.
Back home Mbabazi resumed her role as both mother and caregiver. Ingabire spent part of her early years attending schools for children with disabilities as her health gradually stabilized.
There were periodic complications, routine check-ups and costly medications that continued to strain the family’s modest income. Farming alone could not sustain the mounting needs. Ingabire’s siblings, now older, often contribute financially to support her daily welfare, helping to pay for transport to health facilities, nutritious food and other necessities that protect her fragile health.
Today, Ingabire smiles easily and speaks with quiet confidence. Yet the shadow of her medical history remains. Her condition still requires follow-up consultations and occasional medication.
For the family, access to care is no longer defined by panic over payment. It is safeguarded by Mutuelle de Santé. “When complications come, we go to the hospital knowing we will not be turned away because we cannot pay,” Mbabazi explains.

With Mutuelle de Santé, even those with limited means can access quality treatment and essential medication.
Beyond Policy into People’s Lives
Introduced in the early 2000s, Mutuelle de Santé has grown into the backbone of Rwanda’s universal health coverage, insuring more than 90 percent of citizens. What began as a community-based scheme to remove barriers to primary healthcare has evolved into a national system covering increasingly complex services.
Today, beneficiaries can access advanced orthopaedic procedures, cancer treatment and interventional cardiology, services that were once financially catastrophic for ordinary households.
The system is administered by the Rwanda Social Security Board, which has introduced income-based contributions aimed at reinforcing long-term sustainability. Under the revised structure, the most underprivileged citizens remain fully subsidized, while higher-income earners contribute progressively more.
Policymakers argue that these adjustments are necessary to preserve equity as healthcare costs rise and services expand. For families confronting sudden trauma, the value of that protection becomes unmistakably clear.
Ingabire’s story is far from unique. In September 2021, Roger Uwayezu (not his real name) was involved in a serious accident in Musanze that left him with a fractured thigh. He was later transferred to Kigali for surgery—anxious, despite being insured.
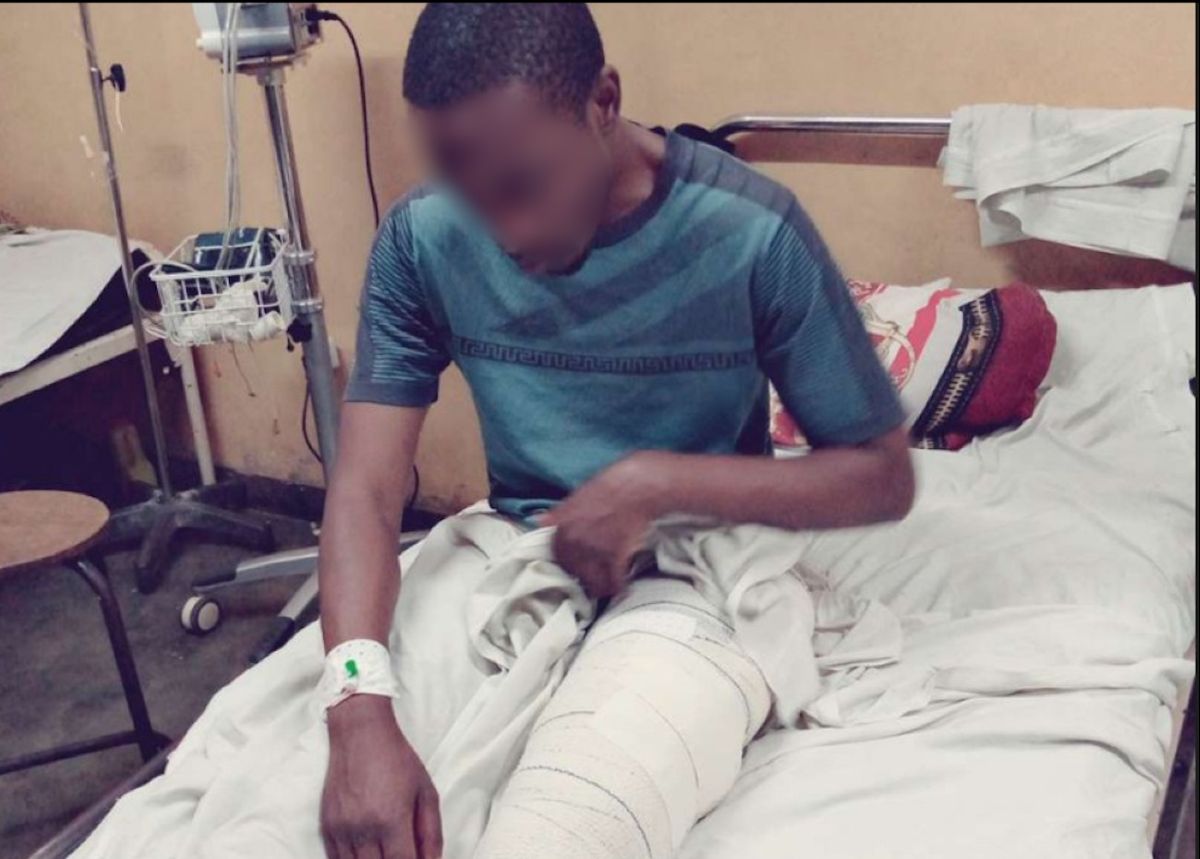
Uwayezu (Not His Real Name) Was Seriously Injured In Musanze And Transferred To Kigali For Surgery. Even With Limited Resources, Middle-Income Earners Can Access Modern Medical Facilities Across The Country.
“Even though I had health insurance, I still wondered how everything would go. I was thinking about how I would manage the bill after discharge,” he recalls.
He underwent surgery and received a metal implant. After several days of recovery, doctors cleared him to return home. In the end, his out-of-pocket costs were less than Rwf 100,000 — compared to nearly Rwf 1 million he would have paid without insurance, a sum difficult to afford on a freelance journalist’s income.
Joseph Manirakiza tells a similar story. Last December, his university-aged nephew was in a motorcycle accident, suffering two major fractures and losing consciousness at the scene. He spent over two months in the hospital, undergoing surgery and beginning physiotherapy before finally being discharged.
A Social Contract Written in Hope
For Ingabire and many others, these stories echo a personal reality. While her major surgery took place abroad years ago, her long-term wellbeing depends on consistent access to Rwanda’s evolving health services.
The expansion of specialized care under Mutuelle strengthens her safety net and reinforces her confidence. “When I feel pain, I don’t panic like before. I know we can go to the hospital,” she says quietly.
Her words illuminate what statistics alone cannot capture. Mutuelle de Santé is more than a financing mechanism; it is a social contract rooted in solidarity. Those with greater means contribute more so that the most vulnerable can receive care without facing financial ruin.
As Rwanda recalibrates contributions to secure the scheme’s future, debates over premiums will inevitably continue. But for families like Ingabire’s, the true measure of reform is not found in spreadsheets.
It is found in a repaired heart that keeps beating, a fractured leg that heals without bankrupting a household, and the quiet dignity of knowing that illness will not mean exclusion.
Understanding the Numbers Behind the Promise
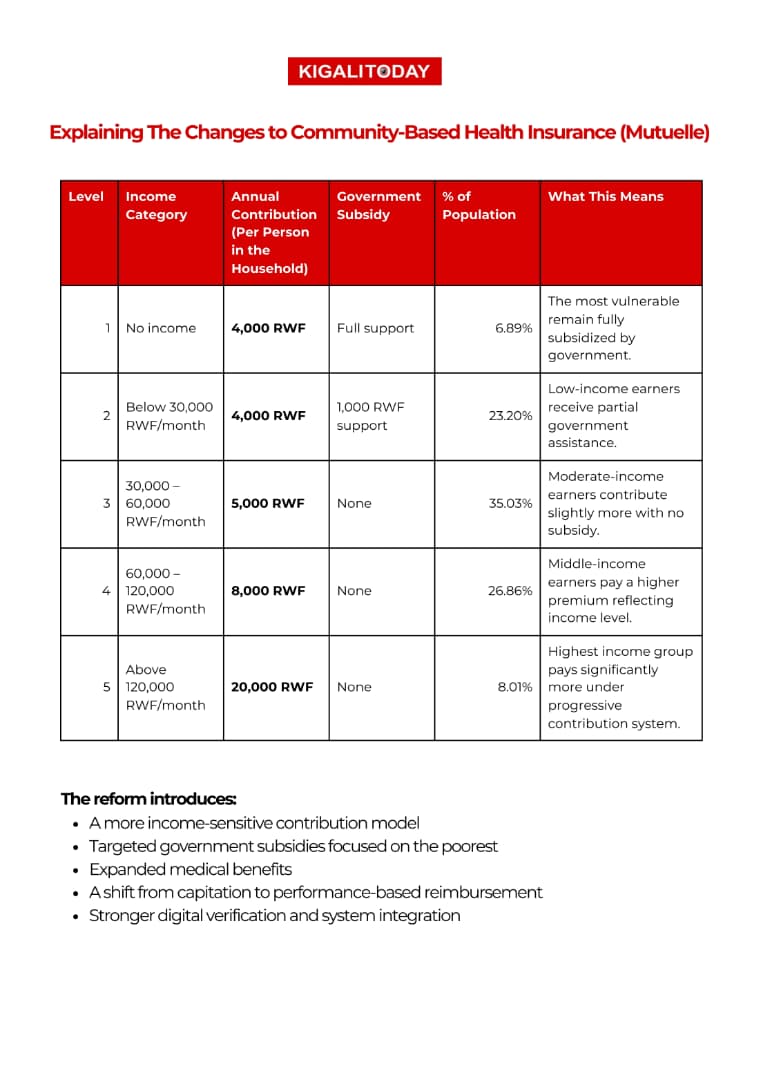
Available data shows that Mutuelle de Santé has expanded steadily over 25 years, with enrollment rising from single digits in the early 2000s to a peak of 91 percent and stabilizing at around 88 percent in recent years.
This sustained coverage reflects strong government backing and broad inclusion of the informal sector. While premiums remained unchanged for over a decade, the benefits package expanded to cover advanced services such as cancer care, dialysis and other non-communicable disease treatments.
In 2024, non-communicable diseases accounted for 47.7 percent of facility deaths and 59.3 percent of community deaths, underscoring the growing demand for long-term care. Per capita expenditure is projected to reach Rwf 13,819 in 2025/26, a 62.7 percent increase compared to the previous year.
The data also indicates that member contributions declined as a share of total revenue, from 67 percent in earlier years to 32 percent in FY 2024/25, increasing reliance on government support.
Together, these figures explain the rationale behind recent premium reforms, aimed at preserving equity while securing the long-term sustainability of Rwanda’s flagship community health insurance scheme.




